That fall day in October 2016 was just like any other weekday. Rich Welmon, a mechanic, got up and went to work; he didn’t think anything of the heaviness he felt in his leg or the short episode of dizziness he experienced during the day. “I thought I was just tired and hungry,” he recalled. “I didn’t worry because there isn’t any history of transient ischemic attacks (TIAs) or stroke in my family.”
But the next afternoon, another episode occurred. Then, at 8:30 p.m. when Rich tried to pick up the television remote control, his left hand refused to function.
“I knew something was wrong,” Rich said. “I wanted to go to the hospital to get checked.”
He was able to get into the car, and his wife, Pauline, drove 10 minutes to the local emergency room in Illinois.
Every Second Counts
Halfway to the hospital, Rich’s left side went numb. “I couldn’t move my left side and knew I’d need help getting out of the car,” he said. “It was scary.”
When he arrived at the hospital, emergency room personnel consulted with Barnes-Jewish Hospital and treated Rich for a stroke by administering tPA, tissue plasminogen activator, through his IV to dissolve blood clots and improve blood flow to his brain.
“Patients who get tPA do better than those who don’t receive the medication,” said Dr. J. Michael Hatlelid, Missouri Baptist Medical Center neurologist and medical director of Stroke Services. “If they are a candidate for the medication, the earlier they can receive it the better.”
“We are thankful that Rich was within the timeframe window to take advantage of tPA,” Pauline added.
Rich was transferred by helicopter across the river to Barnes-Jewish Hospital for more advanced care. Rich spent four days at the hospital where he learned that he had an ischemic stroke caused by a temporary clot in a vessel supplying blood to the thalamus area of the brain.
Choosing the Best Place for Rehabilitation
When it was time to begin rehabilitation, Rich and Pauline decided to move to Missouri Baptist, which was recently recertified by The Joint Commission as a Primary Stroke Center. This Certificate of Distinction recognizes centers that make exceptional efforts to foster better outcomes for stroke care.
“Besides knowing MoBap’s high standard for quality care and the rehabilitation services they offered, we chose the hospital because our daughter is also an occupational therapist there,” Pauline said. “We both wanted family close by while Rich recovered.”
As a primary stroke center, MoBap is prepared to treat strokes and TIAs and help patients recover from these events.
“Our stroke program has grown dramatically,” Dr. Hatlelid said. “We currently treat more than 1,000 patients a year who have suffered strokes. There are new technologies, procedures and standards of care for treating strokes that we use at MoBap.”
Furthermore, the collaboration between MoBap, Barnes-Jewish Hospital and Washington University Physicians brings a high level of care to the community. “We are aggressive with strokes because we want to prevent disability,” Dr. Hatlelid said.
The Road to Recovery
Sara Wilhite, DPT, lead therapist at MoBap, explained that varying levels of care are offered to aid patients in their recovery. “Through one-on-one care we provide individualized treatment based on the patient’s limitations and goals,” she explained. “We offer physical therapy, occupational therapy and speech-language pathology in outpatient and inpatient settings.”
Rich spent 30 days in MoBap’s Acute Rehabilitation undergoing daily physical and occupational therapy. When he first arrived at MoBap, Rich didn’t have any movement on his left side. “Rich worked hard and was motivated,” Pauline said. “Without his determination and compliance with the therapy, he wouldn’t have made the recovery that he did. We’re thankful he’s regained almost all of the function on his left side.”
“I really credit the therapists at MoBap for helping me keep a positive outlook,” Rich said. “They challenged me to reach my goals, but were compassionate at the same time.”
Sara added, “The therapists at MoBap are movement specialists who help patients relearn normal movement patterns after a stroke.”
Rich agreed, “After seeing a sports therapist who focused solely on my muscle strength and then working with the MoBap therapists who are specially trained in stroke recovery, I could see a real difference.”
After he was discharged home, Rich continues to recover and goes to physical therapy at MoBap’s Outpatient Clinic once a week where he focuses on improving his foot drop, gait and muscle strength. He’s also taken advantage of the hospital’s Fitness and Independence Training (FIT) Program where he worked with a certified trainer on an exercise program customized specifically for his needs.
Sara confirmed that within the first three to four months patients usually see the most recovery. “After that recovery slows down, improvement can still be made, even if it’s been a while since the initial event,” she added.
“I've seen patients improve in meaningful ways three to four years after having a stroke,” Dr. Hatlelid added.
Life After the Stroke
Rich acknowledges that life changed after his stroke. He now contends with balance issues and fatigue, as well as mood and emotion changes. Both he and Pauline participate in stroke support groups. One group was formed by MoBap therapists and another through ABC Brigade. Both groups have connected them with others who are going through similar experiences.
Household tasks are also helping Rich recover. “Doing the dishes, vacuuming and brushing our dog, Gertrude, is therapeutic,” he said. “The work has improved my dexterity, balance and coordination and gives me the feeling of contributing to the household.”
After having his stroke, Rich experiences muscle spasms in his left leg. To counteract this, “I get Botox injections into my leg muscles to decrease the spasms and to help with mobility and muscle stiffness,” Rich explained.
Even though he’s experienced plateaus during his recovery, Rich’s outlook is upbeat and positive. “If I have problems doing things, such as getting in and out my truck, working in the garage or tinkering with car models, I simply find ways to adapt my tools, change my way of thinking and overcome the hurdles,” Rich said. “It’s very important to not give up and keep moving forward.”
Be Fast When A Stroke Occurs
Dr. Hatlelid stressed the importance of responding quickly when a stroke occurs. “Many times, people who are having a stroke will ignore the symptoms, not realizing their importance,” he said. “It’s vital to know the risk factors and know the symptoms. Then, if you suspect a stroke, don’t waste time. Call 911. Besides helping patients quickly get to the hospital, they will notify the emergency room before arrival, so staff can prepare medication – like tPA – and other lifesaving interventions.”
Stroke Risk Factors
- High blood pressure
- High cholesterol
- Heart disease
- Diabetes
- Smoking
- Heavy alcohol use
- Physical inactivity and obesity
- Atrial fibrillation (irregular heartbeat)
- Family history of stroke
Stroke Symptoms
Check for any one of these signs which could mean a stroke:
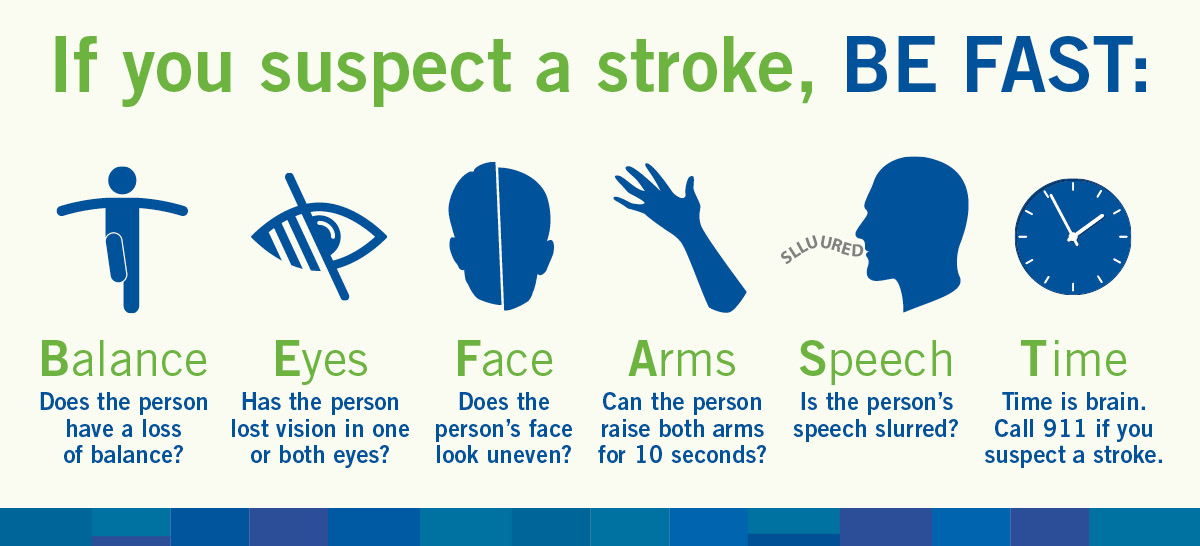
Balance: Does the person have a sudden loss of balance?
Eyes: Has the person lost vision in one or both eyes?
Face: Does the person's face look uneven?
Arm: Is one arm hanging down?
Speech: Is the person's speech slurred? Do they have trouble speaking or seem confused?
Time: Call 9-1-1 now!
Remember to BE FAST and call 911.